Corneal cross-linking is a modern, minimally invasive procedure that helps stabilize and strengthen the cornea in patients with progressive keratoconus or corneal ectasia. This method reinforces weakened corneal tissue to help preserve your vision and potentially delay or eliminate the need for a corneal transplant.
At Richens Eye Center, our eye care services are performed by experienced board-certified ophthalmologists and optometrists. The practice is led by Dr. Sharon Richens, MD, FACS, a board-certified ophthalmologist and Fellow of the American College of Surgeons and the American Academy of Ophthalmology. Dr. Richens and her team serve patients throughout St. George, UT, and Mesquite, NV.
What Is Keratoconus?
Keratoconus, often referred to as ‘KC’, is a non-inflammatory eye condition in which the typically round dome-shaped cornea progressively thins and weakens, causing the development of a cone-like bulge and optical irregularity of the cornea. This causes ‘distortion’ in your vision and can result in significant visual impairment.
Learn more about KC and corneal cross-linking in this short video.
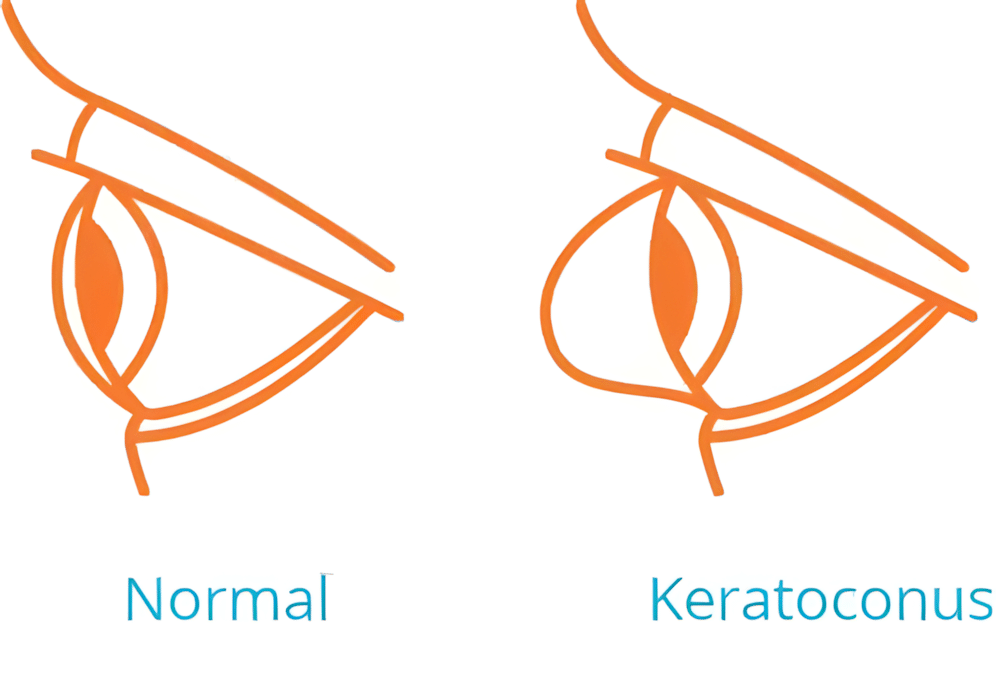
The Symptoms of Keratoconus
Keratoconus typically first appears in individuals who are in their late teens or early twenties, and may progress for 10–20 years, and then slow or stabilize. Each eye may be affected differently. In the early stages of keratoconus, someone may experience:
- Slight blurring of vision
- Distortion of vision
- Increased sensitivity to light
Your cornea is responsible for focusing most of the light that comes into your eye. Therefore, keratoconus or other abnormalities of the cornea can have a major impact on your vision, making simple tasks such as driving or reading very difficult.
In severe cases, keratoconus may result in significant loss of vision and may lead to a corneal transplant.
What Is Corneal Ectasia?
Corneal ectasia or keratectasia, also marked by progressive corneal steepening and thinning, is a rare but serious complication that infrequently follows vision correction procedures—such as laser-assisted in-situ keratomileusis (LASIK) and photorefractive keratectomy (PRK). It is also associated with worsening vision.
What Is Corneal Cross-Linking?
Available at Richens Eye Center, corneal cross-linking is a minimally invasive outpatient procedure that combines the use of UVA light and riboflavin eye drops to add stiffness to the corneal structure that has been weakened by disease or by rare complications after refractive surgery (called corneal ectasia or keratectasia).
Cross-linking has been performed in Europe since 2003 and is now FDA-approved. This procedure is considered the standard of care around the world for keratoconus and corneal ectasia following refractive surgery.
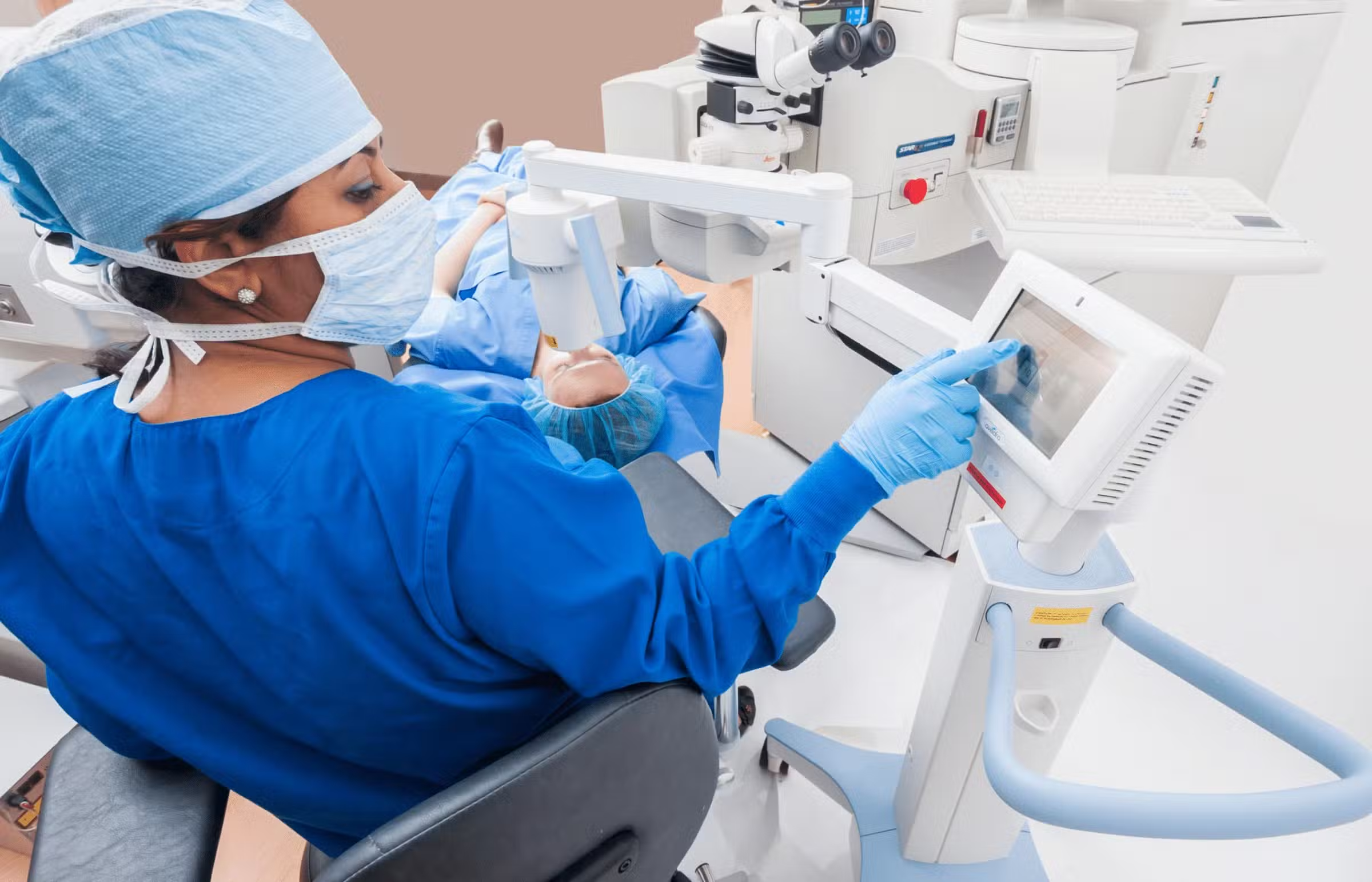
Corneal cross-linking accomplishes the following:
- Creates new corneal collagen cross-links
- Results in a shortening and thickening of the collagen fibrils
- Leads to the stiffening of the
Patient Testimonials
“I was thoroughly impressed with Dr. Richens. She was everything one could hope for in a medical professional: attentive, thorough, professional, and a very skilled communicator. She took the time to listen and diagnose in a way that gave me confidence.”
– Anonymous
“Dr. Richens is amazing! Very professional and very knowledgeable. She is very caring and thoughtful. Gorgeous inside and out! My mom had an emergency and Dr. Sharon Richens made sure that she was in good hands. Thank you so much for recommending Dr. Marcos Reyes. He is amazing! Her surgery was successful. Love Richens Eye Center, St. George Eye Center and St. George Surgical Center! Thanks to all medical professionals who helped us!”
– Anonymous
Riboflavin
Riboflavin (vitamin B2) is important for body growth and red blood cell production, and assists in releasing energy from carbohydrates. Its food sources include dairy products, eggs, green leafy vegetables, lean meats, legumes, and nuts. Breads and cereals are often fortified with riboflavin.
Under the conditions used for corneal collagen cross-linking, riboflavin 5’-phosphate, vitamin B2, functions as a photo enhancer, which enables the cross-linking reaction to occur.
Ultra-Violet A (UVA)
UVA is one of the three types of invisible light rays given off by the sun (together with ultraviolet B and ultraviolet C) and is the weakest of the three.
A UV light source is applied to irradiate the cornea after it has been soaked in the photo-enhancing riboflavin solution. This cross-linking process stiffens the cornea by increasing the number of molecular bonds, or cross-links, in the collagen.
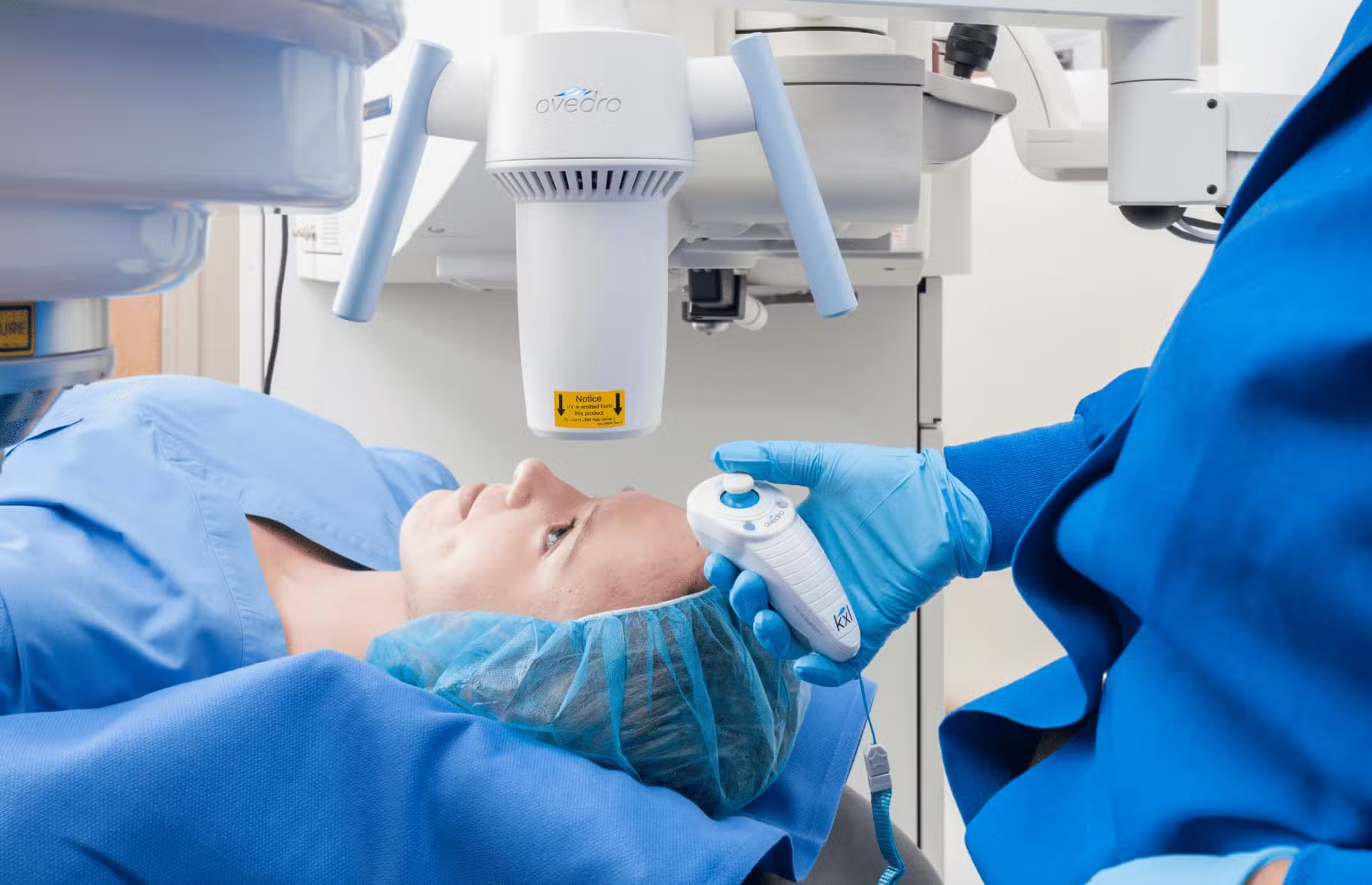
How to Know Cross-Linking Is Right for You
Patients over the age of 14 who have been diagnosed with progressive keratoconus or corneal ectasia should ask their doctor about corneal cross-linking.
We are proud to offer patients in our practice the only therapeutic products for corneal cross-linking that have been FDA-approved to treat progressive keratoconus. This approval offers an effective treatment for patients who, until recently, had no therapeutic options to limit the progression of this sight-threatening disease.
To learn more about keratoconus and the iLink cross-linking procedure, visit Glaukos iLink.
Why Choose Richens Eye Center
Dr. Sharon Richens is a Stanford- and University of Utah-trained board-certified ophthalmologist with a background that includes fellowship training at St. John Ophthalmic Hospital in Jerusalem. Dr. Richens combines clinical expertise with a long-standing commitment to surgical excellence. She serves as adjunct clinical faculty at Rocky Vista University and has earned multiple honors, including Best Resident Research Presentation at West Virginia University and distinction from Stanford’s Honors Program in the Humanities.
Richens Eye Center is also supported by a skilled team of board-certified ophthalmologists and licensed optometrists. This multidisciplinary team brings advanced training and experience in comprehensive eye care, from diagnostics to specialized treatments. As the only provider in Southern Utah to exclusively use all-laser iLASIK rather than traditional blade-based methods, the practice delivers a high level of precision in every treatment plan.
Frequently Asked Questions
Most patients notice some mild discomfort, sensitivity to light, or blurry vision for the first few days after treatment. A soft bandage contact lens is usually placed to protect the cornea while it heals, and prescription drops help prevent infection and reduce irritation.
Vision gradually improves as the eye recovers, with most patients seeing their best results over several weeks to months.
The procedure itself is typically very comfortable thanks to numbing eye drops. Afterward, you may feel some scratchiness or a gritty sensation for a few days, similar to having an eyelash in your eye. Most patients describe it as mild and manageable, and your doctor will recommend ways to ease any temporary irritation while you heal.
Everyone heals at a slightly different pace, but many patients are back to normal activities within three to five days. You may need a little extra time before driving, reading for long periods, or using digital screens comfortably. Your doctor will give you personalized guidance on when it’s safe to return to your regular routine.
Corneal cross-linking is meant to stop or slow the progression of keratoconus or corneal ectasia. Most patients experience stabilization of their vision, which helps preserve long-term eye health. In some cases, vision may even improve slightly as the cornea strengthens and reshapes. Early treatment often provides the best results.
Yes, many insurance plans now cover FDA-approved corneal cross-linking for progressive keratoconus. Coverage for corneal ectasia after LASIK or PRK can vary depending on your provider. Our team can help you confirm your benefits and explain any expected out-of-pocket costs before scheduling treatment.
It’s uncommon to need a second treatment, but it can be done if the cornea shows signs of weakening again. Most patients only need one procedure to maintain corneal strength for the long term, especially when treated early in the disease process.
Corneal cross-linking is very safe when performed by an experienced ophthalmologist using FDA-approved technology. Mild irritation, light sensitivity, and temporary blurry vision are normal during recovery. Serious complications, like infection or scarring, are rare. Your surgeon will review what to expect and how to care for your eyes to ensure the smoothest possible healing process.
Schedule a Consultation Today!
If you’re interested in keratoconus treatment or would like to learn more about corneal cross-linking, contact Richens Eye Center to schedule your appointment. We offer care at four convenient locations:
- St. George/Downtown, UT – Call 435.986.2020
- St. George/Sunset, UT – Call 435.986.2020
- Mesquite, NV – Call 435.986.2020
- Cedar, UT