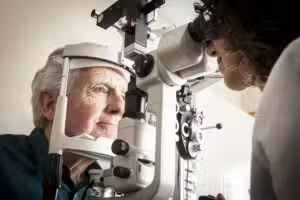
What causes macular degeneration?
Macular degeneration is the result of damage to the nerve cells in the macula. The process that leads to this damage is different for each type.
The dry form is a gradual process. As you age, the cells in the macula start to thin and break down, and waste deposits build up in the back of the eye. Over time, this damages the macula.
The wet form happens when abnormal blood vessels grow in the back of the eye. These blood vessels break easily and leak blood and fluid under the macula. This can quickly damage the macula and distort your central vision. Experts are still studying the causes of both forms, but they know several different things may play a part. You are more likely to have macular degeneration if:
- You are an older adult: The risk of getting macular degeneration increases as you age, starting at around age 50.
- A close family member has macular degeneration.
- You smoke.
- You are white.
What are the types of macular degeneration?
There are two main types of age-related macular degeneration:
Dry Macular Degeneration
By far the most common, the “dry” form of macular degeneration is characterized by the presence of yellow deposits in the macula. These are called drusen. In the early stages, a few small drusen don’t cause vision deterioration. But as they grow in numbers and size, these lead to dimming or distortion of vision that is most noticeable when reading. In the severe stage, patients can develop blind spots in the center of their vision, which can advance to loss of all central vision.
Wet Macular Degeneration
Only about 10 percent of people develop the “wet” form of macular degeneration, but these people make up the majority of those who suffer serious vision loss. The wet form is characterized by the growth of abnormal blood vessels from the choroid underneath the macula. This is called choroidal neovascularization. These blood vessels leak blood and fluid into the retina. This distorts the person’s vision, as straight lines look wavy and blind spots develop. The bleeding of these abnormal blood vessels creates scar tissue that leads to permanent loss of the patient’s central vision.
Symptoms of Macular Degeneration
The main symptom of macular degeneration is dim or fuzzy central vision. Objects may look warped or smaller than they really are. You may have a blank or blind spot in the center of your field of vision. As the disease gets worse, you may have trouble with tasks like reading and driving. The two forms differ in how quickly symptoms develop and how severe they are.
If you have the dry form, your vision will probably become blurry slowly. You may have it for several years before it affects your ability to read, drive, and do everyday activities.
In the wet form, vision loss happens quickly and can be severe. Often the first symptom of the wet form is that straight lines look wavy or curved. If you think you might have wet macular degeneration, see your doctor right away. In some cases, quick treatment may help you keep your central vision.
How is macular degeneration diagnosed?
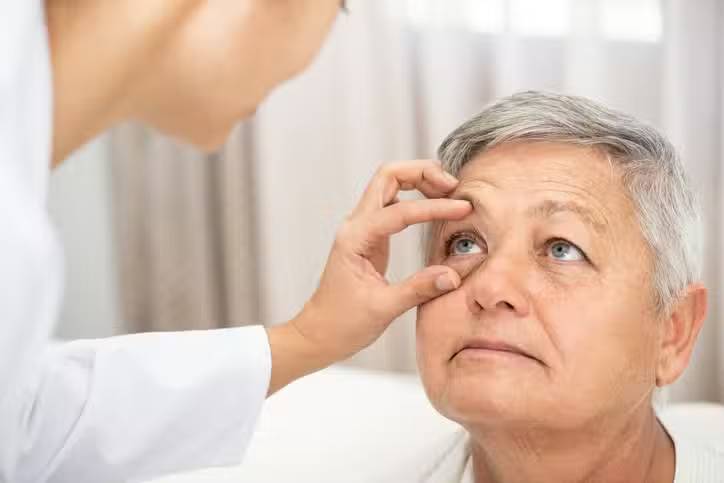
A doctor can usually detect macular degeneration by doing a regular eye exam and asking questions about your past health. You may have some vision tests, including ophthalmoscopy. This test lets your doctor look at the inside of your eye. If you have macular degeneration, your doctor may see drusen. These are yellowish-white waste deposits that can build up at the back of the eye. The doctor may have you look at a chart with lines and a dot at the center.
This is called an Amsler grid. It can help detect changes in your central vision. If you have the wet form, the lines near the center dot will look wavy or curved, or you may see a blank spot or hole in part of the grid.
If you have macular degeneration, your doctor will want to see you for regular follow-up exams. You can also use an Amsler grid at home. Looking at it every day will help you keep track of any changes in your vision.
What our patients have to say
“Very kind and amazing staff, I highly recommend Richens eye center!! Thank you!”
– Karly A.
“Today I was able to witness something amazing here. Had an elderly man I was in care of need some help with his eye and Dr. Tarbet and her staff took care of his eye with such care and was amazing with him. Can’t thank her enough. Also a nice building. All around great experience!!”
– Anonymous
OK, so now that you’ve been diagnosed with age-related macular degeneration, you’ll have lots of questions about your vision. Here are 10 questions you should ask:
Our doctors can give you a good idea by looking at the number and size of drusen if you have the dry form. Injections help control the wet form.
Sometimes, because the focus is the center of the lens, both cataracts and macular degeneration can be behind the deterioration in vision. It’s possible having cataract surgery will help.
Glasses with a high level of magnification, often with built-in prisms, can help by magnifying letters. This is especially helpful for small print.
Certain optometrists specialize in low vision. They help with the optimal magnification in your glasses and can recommend special devices, such as digital magnifiers. Our low vision specialist can help you remain as independent as possible with certain advice and guidance.
Research in age-related macular degeneration is advancing rapidly. See if there is a clinical trial you can get in on.
If you have the dry form, and depending upon the size and number of your drusen, it can help to take AREDS2 vitamins.
Some patients require monthly injections to maintain their best vision, but others may be able to do fine with less frequency.
The vision loss with macular degeneration will mean loss of driving eventually. The question is — what are the signs I need to watch for as clues to when I should be done?
Siblings and children of people with age-related macular degeneration have approximately twice the risk of also developing the disease. Ask what steps you can educate them about to reduce their risk.
Our doctors will have you perform various vision checks at home to detect any new onset of wet macular degeneration. Ask for what new symptoms deserve attention.
Schedule a Consultation
To schedule a consultation, or to learn more about our Macular Degeneration procedures, contact us or click below to call or text us today! Our practice serves St. George, UT & Cedar, UTand the surrounding areas.